VERTEBRAL
EMBOLIZATION
ANATOMY
If the arterial vascularisation
of the osseous and muscular envelopes of spinal cord is rich since it comes
from multiple metameric arteries, the arteries of the spinal cord which
are rather delicate, are a different case in point.
Indeed, the whole of the spinal cord
is fed by only 6 or 8 anterior radiculo-medullary arteries
(leading to1 anterior spinal axis) and a score of posterior radiculo-medullary
arteries (leading to the postero-lateral spinal axes). The provision
of vascularization of the osseous envelopes and musculo-ligaments of spinal
cord is simpler since only two cervical and dorso-lumbar areas can be distinguished.

CERVICAL AREA:
At this level, vertebro-medullary
vascularization is ensured by the ascending branches of the right and left
subclavian arteries : lower thryoidian artery, ascending cervical artery,
depp vertebral and cervical artery.
These are organized in 3 axes : 1
/ anterior cervical or pre-vertebral ( lower thyroidian and mid cervical
ascending artery) / latero-vertebral (vertebral) and / posterior (cervical
deep).
These 3 axes are largely anastomosed
between each other by peri-vertebral horizontal or intrarachidian ramus
which ensure the vascularization of the vertebrae.
Thus, the vascularization of the
body of the cervical vertebrae is ensured by branches coming from the thyroid
arteries, the ascending and vertebral cervicals arteries and the posterior
arc through the deep vertebral cervical arteries.
It is at the cervical level that
the anterior spinal axis receives the most afferent arteries (13 to 4).

Anterior
cervical spinal artery
- the radiculo-medullary artery does
not usually exist in the high cervical area (C1 to C3)
and the afferents to the anterior
spinal axis come from the joining of 2 spinal arteries developing from
the end of each vertebral artery.
- at the mid and lower cervical level
the anterior spinal axis is fed by 2 to 4 anterior radiculo-medullary arteries
developing indifferently on the right or the left of the vertebral artery
or the deep cervical artery, or exceptionally from the ascending cervical
artery or directly from the subclavian artery.
Generally, there are 2 principal
radiculo-medullary arteries, one developing from the vertebral artery compared
to the C5-C6 or C4 -C5 lateral foramen and an an artery developing from
the deep cervical artery and penetrating into the rachidian channel through
the C7-D1 lateral foramen.
This artery ensures the vascularization
of the cervical spinal cord but can be replaced by a radiculo-medullary
artery coming from the vertebral and satellite artery of the 6th cervical
root.
The posterior spinal axes are spindly
and are fed by 4 to 6 very fine posterior radiculo-medullary arteries coming
from the vertebral artery between C3 and C6. At this level, the possibilities
of substitution in the event of occlusion of one of the radiculo-medullary
arteries are generally good, the rarity of medullary accidents observed
at the time of atheroma or therapeutic occlusions of the vertebral artery.

DORSAL
AND LUMBAR AREA
The vascularization of the rachis
and spinal cord is ensured by the intercostal arteries and lumbar exiting
in pairs from the dorsal face of the aorta.
1-VASCULARIZATION
OF THE RACHIS:
On the vascular level, the vertebrae
also consist of two distinct parts : the vertebral body and the posterior
arc.
-
VASCULARIZATION OF BODY VERTEBRAL:
The vertebral body is fed by two arterial
groups. The anterior group is formed of multiple small periostic branches
coming from the trunk of the intercostal artery which vascularize
the peripheral portion of the anterior and lateral sides of the vertebral
body.
The posterior group providing the
majority of the vascularization of the vertebral body, comes from the anterior
branch of the rachidian tract (retro-corporal artery), via 2 perforating
branches which penetrate the vertebral body through its vascular hilum
whose branches vascularise the posterior side of the vertebral body, and
most of the central-corporal region.

-
COSTO-VERTEBRAL VASCULARIZATION :
It is fed by branches coming from the
anterior branch of the inter-costal artery, the two branches coming from
the dorso-spinal artery during its passage through the para-vertebral space.
-VASCULARIZATION
OF POSTERIOR ARC :
This also receives a double intra-tract
supply through branches situated in the posterior epidural space (pre-mammary
artery) coming from the posterior intra-tract branch of the
dorso-spinal artery.
It also receives periostite extra-rachidian
afferents coming from the internal branch of the divisions of the dorso-spinal
artery endings.

2-VASCULARIZATION
OF SPINAL CORD:
If the provision of the vascularization
of the rachis is identical on the whole to that of the dorsal and lumbar
rachis, it is different to the vascularization of spinal cord where it
is necessary to distinguish after Lazorthes, two distinct upper and middle
dorsal and dorsal-lumbar regions .
-Upper
and middle dorsal (D3 to D7):
This This region is thus characterized
by its poor vascularity and therefore its greater fragility. In all
this area, there is only one anterior radiculomedullary artery. It usually
comes from the posterior dorso-spinal branch of the 4th or 5th intercostal
artery, more often on the left ( in 80 % of cases) than on the right.
The posterior radiculo-medullary
arteries are themselves little developed and vary in number, from 4 to
9.
They come from the dorso-spinal
branch of the intercostal artery, after the crossing of the nerve root,
skirt its posterior face, then cross the dura mater and move up and inside
to the posterior collateral sulcus where they join the posterior spinal
axis.
The frequent existence of a common
trunk of the 4th and 5th intercostal right artery and the bronchial artery
of the lower right lobe must be pointed out.
In certain cases, this trunk can
provide the anterior radïculo-medullary artery of the dorsal segment
and this anatomical provision is certainly responsible for neurological
complications which could be observed with the waning of embolization
of the bronchial arteries.
Lastly, when speaking about anatomical
variations, it is necessary to point out the possibility of partial or
total vascularization of the upper dorsal region by branches of the sub-clavian
artery.

-DORSO-LOMBAR
TERRITORY:
At this level, vertebro-medullary vascularization
has the same form as at the upper dorsal level, the intercostal and lumbar
arteries are often bulkier and their anastomoses more developed, in particular
at the lumbar level.
The anterior spinal axis generally
receives a single afferent, the bulky Adamkiewicz artery, which ensures
the major part of the vascularization of lower dorsal spinal cord and of
the conus.
In 70% of cases, the artery originates
on the left side and in 80 % of cases is formed between D9 and L2.
When its origin is located on
a low level, below D12, an anterior middle dorsal radiculomedullary artery
is often found, coming from the 7th or 8th intercostal artery. It is not
exceptional, in particular in children or the adults, to observe
the presence of one or two extra , anterior radiculo-medullary arteries
in the lower dorsal area.
The posterior radiculo-medullary
arteries (posterior spinal) are well developed at this level, and between
4 and 8 can usually be counted. Two of them, which are more developed,
are constant : these are the posterior spinal arteries of the cone. They
usually emerge between D12 and L3 and are anastomosed with the ending of
the Adamkiewicz artery to form the anastomotic conus arteriosus.

Anterior spinal
artery and anasomoses at risk
Finally, the presence of very
spindly radicular arteries, satellites of the lumbar roots, which
could provide for the vascularization of the final cone in the event of
occlusion of the Adamkiewicz artery, must be pointed out.

VEINS:
There are very few studies concerning
the medullary venous return.
Their anatomical position approaches
that of the arteries : indeed, the intramedullary veins run into the anterior
and posterior peri-medullary plexus. These drain into medullary-radicular
veins and, from there, into the intrarachidian plexuses.
MEDULLARY
VENOUS NETWORK
This is made of central veins
which present a radiating position and run directly or via horizontal peri-medullary
veins into 2 principal veins, the anterior spinal vein and the posterior
spinal vein , whose gauge and tract are very variable, however the most
frequent position deserves mention :
- the anterior , median and rectilinear
spinal vein, leads into the anterior middle sulcus and drains the front
quarter of spinal cord. This vein appears to be continuous from the cephalic
extremity to the caudal extremity of the spinal cord ;
. - the posterior spinal vein
is sinuous and follows both sides of the centre line, its gauge is more
significant than that of the forementioned vein and it is often bulkier
at the level of the lumbar or cervical bulge. Lastly, it should be noted
that this vein can be duplicated in the cervical area. This vein drains
the back three-quarters of spinal cord.

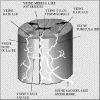
Diagram
and description of the perimedullary venous networks
EFFERENT
VEINS
These are formed from a varying number
of the anterior and posterior medullary-radicular veins. Usually, there
are 2 or 3 medullary-radicular veins in the cervical area, one at the upper
dorsal level, one at the middle dorsal level, 2 at the level of the cone
and 1 in the lumbar area ( filum vein). These veins run into the intrarachidian
plexuses in comparison with the lateral foramen.

EMBOLIZATION
MECHANISM
The aim of vertebral embolization
is to significantly reduce hypervascularisation related to
the angiogenesis of tumoral origin.
The appearance of one tumoral necrosis
results from embolization if all the pedicles taking part in
neovascularization are treated.
The interest is threefold :
It can allow, through the reduction
of bleeding during the operation, for an easier handling of
certain primitive hypervascular tumours
of the rachis or of hypervascular metastases (kidney, thyroid...),
by significantly reducing the bleeding of these lesions during the operation.
Through the tumoral necrosis that
it leads to, embolization results in a reduction in the mass
compression brought about by tumoral invasion and sometimes allows for
a partial or complete lifting of a nervous compression beyond the reach
of other therapeutic resources like surgery or radiotherapy.
Finally and undoubtedly related to
the two forementioned mechanisms, embolization can significantly
attenuate the vertebral pains related to tumoral invasion.
One can, in certain circumstances,
in particular for secondary lesions which are not numerous (one or two),
and of a slow evolution, associate an intra-arterial local chemotherapy
by carrying out a chemoembolization . The interest of chemotherapy in this
case for lesions considered to be chemosensitive is to locally bring a
significant concentration of alkylant type cytostatics or anthracyclines
within the tumour using weak concentrations compared to the amounts
injected for an intravenous treatment.
This leads to a better clinical tolerance
and a reduction in side effects particularly effects on full blood count.
It should be remembered that the intra-arterial administration of cytostatic
must come within the framework of procedures which have already been used
and after multidisciplinary consultation since this treatment falls outside
the scope of the AMM for the products mentioned.

TECHNIQUE
This technique is common to the
diagnostic vertebromedullary angiography and thus shares these main principles.
Thus it relies on a perfect knowledge
of the arterial and venous vertebromedullary vascular anatomy.
The advantages, the drawbacks and
the risks of this technique will have been explained to the patient beforehand.
An assessment of clotting time, a
full blood count and an ionogram are essential to avoid all risks of bleeding
and renal insufficiency, considering the volume of iodine injected, and
to ensure the absence of red or white blood cell depletion before a possible
chemoembolization .
Of course if necessary medication
to prevent any allergy will have been given beforehand.
The examinations are preferably carried
out under neuroleptanalgesy.
The catheterization is usually done
by a femoral artery way (seldinger) and an initiator adapted to the gauge
of the catheter is used (5F generally). This initiator allows for catheter
to be changed, something which can sometimes be frequent considering the
variations in the access to the intercostal or lumbar arteries.
The length of the treatment leads
to the use of a continuous system of rinsing the initiator and of any coaxial
system introduced into the patient's vascular network at the risk of embolic
migration or occlusion of the carrying catheter in particular the
microcatheters.
An angiographic cartography is highly
desirable with the aim of locating the anterior or posterior spinal
artery before any embolization treatment.
The principle of STABILITY of the
catheter on the level of an intercostal or lumbar is fundamental in avoiding
any migration of occlusion particles towards the aorta and its branches.
Thus the choice of the catheter is
adapted to the shape of the catheterized vessels to ensure an introduction
of the catheter well beyond the arterial ostium. If the catheterization
remains limited a microcatheter will be used to reach the distality of
the artery to be embolised.
Catheter-artery
adequacy
It is imperative to respect the anterior
and posterior radiculo-medullary arteries.
Once in place a high quality angiography
is carried out to check one final time the absence of arterial branches
destined for the spinal cord or dangerous anastomosis.
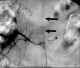
Dangerous
anastomoses
After each sequences of embolization
an angiographic control is necessary in order to eliminate the appearance
of dangerous anastomoses which can appear with the disappearance of the
phenomenon of theft of tumoral hypervascularization. It is often necessary
of embolize both sides as well as the levels just above and just under
considering transverse and cranio-caudal anastomoses.

MATERIEL
The The catheter used must be
adapted to the configuration of the branches being catheterized.
The most commonly used are those
known as COBRA which can have various curves (type I, II, III). For
the low lumbar arteries and the branches destined for the rachidian of
the hypogastric artery, the counter curve of the catheter can be used to
transform them into SIMMONS.

Catheter
Microcatheters are sometimes essential
if you want to avoid any risk of backward flow.
The Mag 2F-3F replaced recently by
Magellan can be quoted.
The most used occlusion agents are
particles of Ivalon (ultra Drivalon) gauged into 150 -250, 250-500 microns,
Embospheres and sometimes free coils (to treat a carrier trunk).
Digitalization is interesting because
it gives a very good quality of imagery by subtraction, and reduces
the amounts of iodine tracer injected, with a reduction of the time of
the examination.

COMPLICATIONS
Complications are slight when
the treatment is carried out by experienced hands, since the major
risk is the embolization of an artery destined for the spinal cord
and the precautions mentioned previously fortunately mean that this
risk is rare.
The other complications are in connection
with the point of puncture like a hematoma or the femoro-femoral arteriovenous
fistula.
INDICATIONS
The indications must be given within
the framework of multidisciplinary meetings bringing together cancer specialists,
radiotherapists, surgeons and radiologists.
They concern secondary hypervascular
lesions like metastases of thyroid cancer, renal cancer, melanomas or of
pheochromocytomas.
Clinical
case :embolization of metastases
They can also relate to primitive
lesions considered to be hemorrhagic during surgical approach (Tumours
with giant cells, vertebral angiomas, benign osteoblastomas , aneurismal
bone cysts).
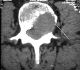
Clinical
case :embolization of lumbar metastases (2)
The goal of the angiography is to
indicate the hypervascularization, to locate the anterior spinal axes and
to allow the embolization to finally be carried out.
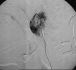
Clinical
case: embolization of a cervical metastasis

|






